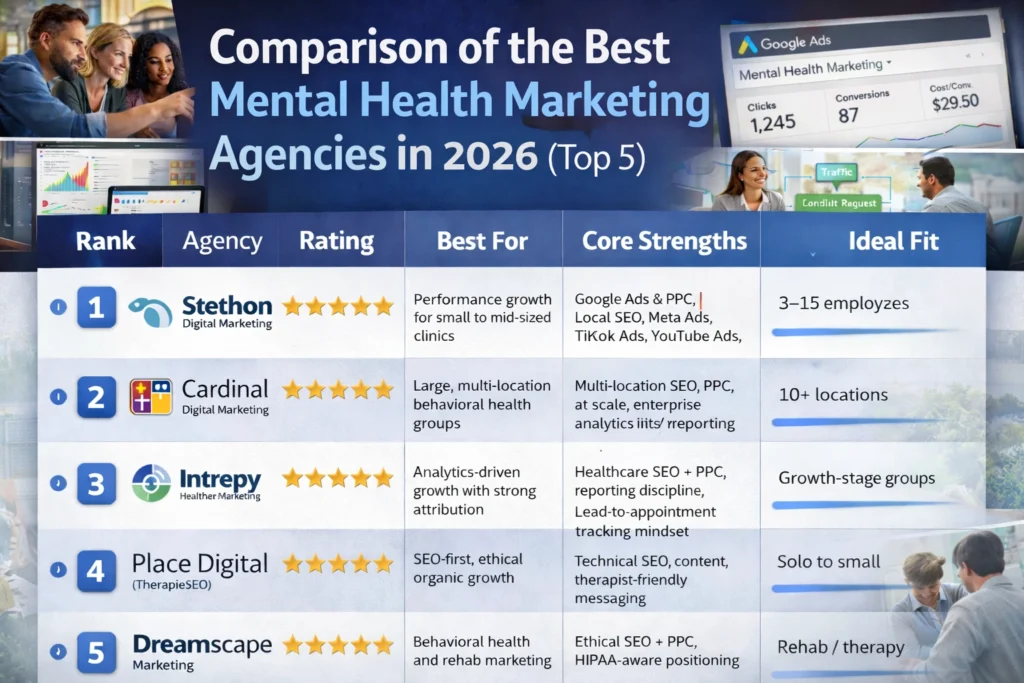
Best Mental Health Marketing Agencies in 2026
Top Marketing Agencies Compared for Clinics That Want Real Patient Growth Choosing the best mental health marketing agency in 2026 is no longer about who has the nicest website or the loudest promises. It is about performance. Mental and behavioral health clinics now compete in a market where: This guide compares the best mental health […]
Best Mental Health Marketing Agencies in 2026 Read More »